“I have Plantar Fasciitis and Doctor was very patient with me, providing exercise and answers to all my questions and I am now seeing improvement for the first time in months.”Google reviewer · Google
“He finally freed me from my plantar fasciitis! Orthotics he casted for me are something exceptional.”Google reviewer · Google
“For nearly fifteen years, I have seen countless foot doctors for pain in my foot. Dr. Patish's diagnosis was dead on. He was the only doctor that got it right.”A. Holston · Google
“Dr Patish and his staff are great! I've gone in with mainly plantar fasciitis… he helped immensely! Knowledgeable in many areas.”Google reviewer · Google
“He is amazing… tells me what is really wrong… truly cares.”Healthgrades reviewer · Healthgrades
“Totally my kind of doctor — tiny office, lots of time, lots of good questions, and a GREAT personable, droll man.”Google reviewer · Google
“I have Plantar Fasciitis and Doctor was very patient with me, providing exercise and answers to all my questions and I am now seeing improvement for the first time in months.”Google reviewer · Google
“He finally freed me from my plantar fasciitis! Orthotics he casted for me are something exceptional.”Google reviewer · Google
“For nearly fifteen years, I have seen countless foot doctors for pain in my foot. Dr. Patish's diagnosis was dead on. He was the only doctor that got it right.”A. Holston · Google
“Dr Patish and his staff are great! I've gone in with mainly plantar fasciitis… he helped immensely! Knowledgeable in many areas.”Google reviewer · Google
“He is amazing… tells me what is really wrong… truly cares.”Healthgrades reviewer · Healthgrades
“Totally my kind of doctor — tiny office, lots of time, lots of good questions, and a GREAT personable, droll man.”Google reviewer · Google
“I have Plantar Fasciitis and Doctor was very patient with me, providing exercise and answers to all my questions and I am now seeing improvement for the first time in months.”Google reviewer · Google
“He finally freed me from my plantar fasciitis! Orthotics he casted for me are something exceptional.”Google reviewer · Google
“For nearly fifteen years, I have seen countless foot doctors for pain in my foot. Dr. Patish's diagnosis was dead on. He was the only doctor that got it right.”A. Holston · Google
“Dr Patish and his staff are great! I've gone in with mainly plantar fasciitis… he helped immensely! Knowledgeable in many areas.”Google reviewer · Google
“He is amazing… tells me what is really wrong… truly cares.”Healthgrades reviewer · Healthgrades
“Totally my kind of doctor — tiny office, lots of time, lots of good questions, and a GREAT personable, droll man.”Google reviewer · Google
“I have Plantar Fasciitis and Doctor was very patient with me, providing exercise and answers to all my questions and I am now seeing improvement for the first time in months.”Google reviewer · Google
“He finally freed me from my plantar fasciitis! Orthotics he casted for me are something exceptional.”Google reviewer · Google
“For nearly fifteen years, I have seen countless foot doctors for pain in my foot. Dr. Patish's diagnosis was dead on. He was the only doctor that got it right.”A. Holston · Google
“Dr Patish and his staff are great! I've gone in with mainly plantar fasciitis… he helped immensely! Knowledgeable in many areas.”Google reviewer · Google
“He is amazing… tells me what is really wrong… truly cares.”Healthgrades reviewer · Healthgrades
“Totally my kind of doctor — tiny office, lots of time, lots of good questions, and a GREAT personable, droll man.”Google reviewer · Google
Posterior Tibial Tendon Dysfunction
Your rehabilitation guide for posterior tibial tendon dysfunction — evidence-based exercises to reduce pain and restore function.
At a glance: The posterior tibial tendon is the main cable supporting your medial arch. When it becomes inflamed or degenerates from overuse, the arch gradually flattens and the foot rolls inward. PTTD is the most common cause of adult-acquired flatfoot. Caught early (Stage 1-2), it responds well to exercises, orthotics, and bracing. Left untreated, it can progress to rigid flatfoot that may require surgery.
⚠️ See Dr. Patish Before Starting Exercises
This condition can involve structural damage that requires professional evaluation. Even mild pain can be a sign of a more serious injury that could get worse with exercise. Please call (760) 728-4800 to schedule an evaluation before beginning this exercise program.
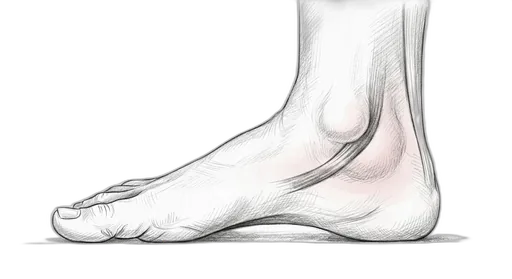
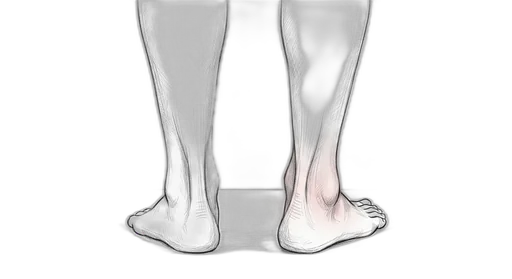
Understanding Posterior Tibial Tendon Dysfunction (PTTD)
Your posterior tibial tendon runs from deep in the calf, behind the inner ankle bone, and attaches to several bones in the midfoot. Every time you push off during walking, this tendon locks the midfoot joints and lifts the arch — it's essentially the winch that holds your foot together during weight-bearing. When the tendon is overstressed — from obesity, high-impact activity, or simply years of unsupported flat feet — it begins to stretch and weaken. As it elongates, the arch drops, the heel tilts outward, and the forefoot splays. The exercises in this program focus on strengthening the intrinsic foot muscles that can take some of the load off the posterior tibial tendon, essentially building a second line of arch support from the inside.
Common Symptoms
- Pain and swelling along the inner ankle and arch
- A gradual flattening of the arch on one side
- The heel tilting outward when viewed from behind
- Difficulty standing on tiptoe on the affected side
- Pain that worsens with activity, especially walking or standing for long periods
The Walking Self-Test
Before you begin any exercises, this simple self-test shows you what your feet are actually doing when you walk. Most of us have no idea — we just walk. But your feet may have quietly developed blind spots: parts of the sole that don't engage anymore, toes that don't push off, or an arch that has checked out. This test takes 60 seconds and gives you a personal baseline you can revisit after each week of exercises to feel your progress.
How to do it: Take off your shoes and socks. Walk slowly across a room — about 10 steps. Pay close attention to each step and notice: Does your heel land first, or does your whole foot slap down at once? As your weight moves forward, do you feel it roll through your arch? Do all five toes engage and push off at the end of the step, or do some of them just ride along? Is one foot doing more work than the other? Don't try to "fix" anything — just notice. That awareness is the starting point. Repeat this test after one week of doing your exercises. Most patients are surprised by how much they can feel changing.
Do this before your very first exercise session, then repeat it once a week. It's your personal progress tracker — no equipment, no numbers, just awareness. Many patients tell us this simple test was the moment they realized their feet weren't working the way they thought.
How to Monitor Pain During Exercise
Use a 0–10 scale to rate your pain during exercise, where 0 is no pain and 10 is the worst imaginable.
Which Level Should I Start At?
Pain ≤3 out of 10 at rest. You're walking normally. Daily activities are manageable with minor discomfort.
Pain 4–6 out of 10. You might be limping or avoiding certain activities. Some things you used to do easily are now uncomfortable.
Pain 7+ out of 10. Walking is difficult. You may need to hold onto furniture or avoid standing altogether.
Start With These Exercises
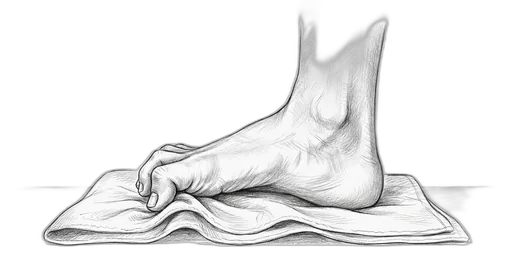
Towel Curl
This exercise strengthens the small muscles on the bottom of your foot — called the intrinsic foot muscles. These are the muscles that support your arch from the inside, kind of like a built-in orthotic. When they're strong, they help distribute your body weight more evenly, protect against overpronation (your foot rolling inward too much), and take stress off the plantar fascia, tendons, and joints.
What to expect: You may not feel dramatic changes in the first few weeks, but stick with it — these small muscles take time to build. By 6–8 weeks, many patients notice better arch support, less foot fatigue at the end of the day, and improved balance. The research shows measurable strength gains by 4–6 weeks.
How to do it: Sit in a chair with your bare feet flat on the floor. Lay a small towel flat under your foot. Curl your toes to scrunch the towel toward you — like you're trying to pick it up with your toes — then spread your toes flat and repeat. Try to use all five toes, not just the big one.
| Level | Hold | Reps | Sets | How Often | Tips |
|---|---|---|---|---|---|
| Mild | 3–5 sec per curl | 10 | 3 | 1×/day | Focus on curling with all your toes evenly — it takes practice, and that's okay |
| Moderate | 3 sec per curl | 8 | 2 | 1×/day | Use a thin towel on a smooth floor to make it easier |
| Severe | 2 sec per curl | 5 | 1 | 1×/day | If the towel is too hard, just practice curling your toes on carpet without it |
How to progress: Start with a thin towel on a smooth floor → thicker towel → place a small water bottle at the far end of the towel for added resistance. When seated feels easy, try it standing.
⚠ When to skip this: Hold off if you're recovering from hammertoe surgery or an acute plantar plate tear (first 4 weeks). Your surgeon will let you know when it's safe to start.
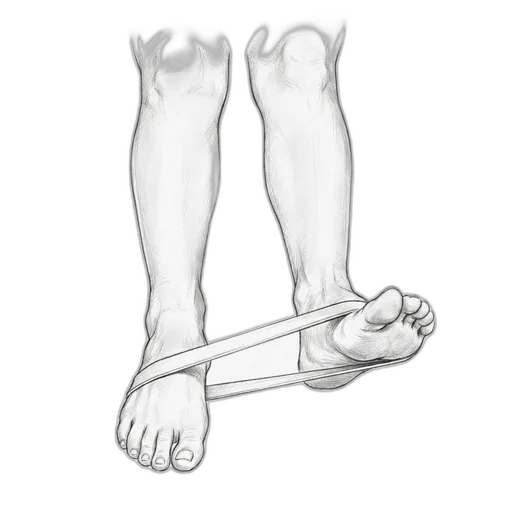
Resistance Band Eversion
This exercise strengthens the peroneal muscles — the muscles on the outside of your lower leg that prevent your ankle from rolling inward. Think of them as your ankle's natural brace. After a sprain, these muscles often weaken and their reflexes slow down, which is a big reason why people re-sprain the same ankle. Resistance band training rebuilds that strength and re-trains the "catch reflex" that protects you.
What to expect: By 4–6 weeks, your ankle should feel noticeably more stable during walking and on uneven surfaces. Strength testing typically shows meaningful improvement by 6 weeks. The real win: a significantly lower chance of re-spraining your ankle — studies show up to 50% reduction in re-injury with consistent peroneal training.
How to do it: Sit with your legs out in front of you. Loop a resistance band around the ball of your foot and anchor the other end to something sturdy (a table leg works well) or your other foot. Slowly turn the sole of your foot outward against the band's resistance, then return slowly. Keep your knee still — the movement should come from your ankle, not your leg.
| Level | Hold | Reps | Sets | How Often | Tips |
|---|---|---|---|---|---|
| Mild | 2 sec at end range | 15 | 3 | 1×/day | Use a medium band. Go slow: 3 seconds out, 2-second hold, 3 seconds back. Control matters more than speed |
| Moderate | 2 sec at end range | 10 | 2 | 1×/day | Use a light band. Slow and smooth — don't let the band snap your foot back |
| Severe | 1 sec at end range | 8 | 1 | every other day | Use the lightest band you can find. Stay in a pain-free range. If your ankle swells after, ice it and rest a day |
How to progress: Light band → medium → heavy. Once eversion is solid, add inversion (turning inward) and dorsiflexion/plantarflexion (up and down) to work all four directions. The ultimate progression: standing on one leg while doing band work.
⚠ When to skip this: Wait at least 72 hours after an acute ankle sprain before starting. Don't do this if you have a peroneal tendon that's subluxing (popping out of its groove) — that needs to be addressed first. Post-surgical: wait until Dr. Patish clears you.

Single-Leg Balance
This is proprioception training — teaching your ankle to "know where it is" in space. After a sprain or injury, the tiny nerve sensors in your ligaments and tendons get damaged, which means your brain doesn't get accurate information about your ankle position. That's why the ankle feels "wobbly" or "unreliable." Balance training rewires those nerve connections and retrains the fast-twitch muscle reflexes that catch you before you roll your ankle. It's like physical therapy for your nervous system.
What to expect: You'll probably wobble a lot at first — that IS the exercise working. By 2–3 weeks you should be able to stand for 30 seconds without touching the wall. By 6 weeks, research shows significantly improved ankle stability and a 35–50% reduction in re-sprain risk. That's the kind of protection that lasts.
How to do it: Stand barefoot on one leg near a wall or kitchen counter — close enough to catch yourself if you need to. Keep the standing knee slightly soft (not locked), look straight ahead, and try to hold your balance without touching anything. It's okay to wobble. It's okay to touch the wall. That's the process.
| Level | Hold | Reps | Sets | How Often | Tips |
|---|---|---|---|---|---|
| Mild | 30 sec | 3 | 1 | 1×/day | Once 30 seconds is easy with eyes open, try closing your eyes. Then try standing on a pillow. Add arm movements or turn your head side to side for an extra challenge |
| Moderate | 20 sec | 3 | 1 | 1×/day | Eyes open only. Touch the wall when you need to — there's no shame in it. The wobbling IS the training |
| Severe | 10 sec | 5 | 1 | 1×/day | Keep two fingertips on the wall if needed. Wear shoes if barefoot is too painful. Progress to no touch when you're ready |
How to progress: Hard floor → foam pad → folded pillow → BOSU ball. Eyes open → eyes closed (much harder!). Standing still → catching and throwing a ball → having someone gently push your shoulder.
⚠ When to skip this: Don't do single-leg balance if you're non-weight-bearing (fracture recovery). Skip during active vertigo or dizziness. Wait at least 1 week after an acute ankle sprain before trying this.
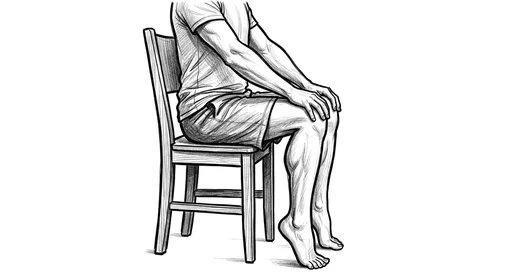
Seated Heel Raise
This is a gentle way to start strengthening your calf and Achilles tendon without putting your full body weight through them. Because you're sitting, the load on the tendon is much lower — which makes this a great starting point if standing exercises are still too painful. It mainly targets the soleus muscle and begins the process of tendon loading, which is how tendons heal and get stronger (they actually need controlled stress to remodel and repair).
What to expect: This is your stepping stone to the more challenging standing exercises. Within 2–3 weeks you should notice you can do more reps with less discomfort. When you can comfortably do 3 sets of 15 with hand pressure on your knees, you're ready to progress to standing heel raises.
How to do it: Sit in a sturdy chair with your feet flat on the floor, about hip-width apart. Place your hands on top of your knees — they'll add a little resistance. Raise both heels off the floor as high as you can, hold briefly at the top, then lower slowly. Think "slow elevator going up, even slower coming down."
| Level | Hold | Reps | Sets | How Often | Tips |
|---|---|---|---|---|---|
| Mild | 2 sec at top | 15 | 3 | 1×/day | Press your hands into your knees for added resistance. 2 seconds up, 2-second hold, 3 seconds down |
| Moderate | 2 sec at top | 10 | 2 | 1×/day | Hands resting lightly — no pressing. Slow and controlled |
| Severe | 1 sec at top | 8 | 1 | every other day | Both feet together. Stop if heel pain gets worse during or after |
How to progress: Both feet → single leg. Add weight by placing a heavy book or dumbbell on your knee. When 3×15 single-leg with added weight is comfortable, you're ready for standing heel raises and eventually step eccentrics.
⚠ When to skip this: Skip during acute calcaneal (heel bone) fracture, active gout flare, or the first 2 weeks after Achilles surgery.
Add These When Ready
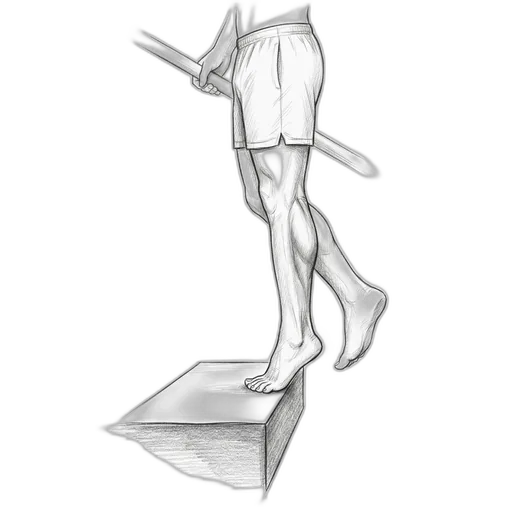
Step Heel Raise (Eccentric)
This is the heavy hitter for Achilles tendon rehabilitation. The eccentric phase — the slow lowering of your heel below the step — is where the magic happens. When you lower under load, it stimulates the tendon to remodel and repair itself at the cellular level. This is based on the Alfredson protocol, which has the strongest evidence of any exercise for Achilles tendinopathy (tendon damage from overuse). It's not comfortable at first — mild to moderate pain during the exercise is actually expected and acceptable — but it works.
What to expect: This is a 12-week commitment, and that's important to understand upfront. Most patients start feeling improvement around weeks 4–6, with significant gains by 12 weeks. At 5-year follow-up, this protocol shows lasting results. The goal is to get back to your normal activities without that nagging tendon pain.
How to do it: Stand on the edge of a step or stair with the balls of your feet on the step and your heels hanging off the edge. Hold a railing for balance. Rise up on BOTH feet (this is the easy part), then shift your weight to the affected leg and SLOWLY lower your heel below the step level — count to three on the way down. Use your good leg to push yourself back up. Don't use the affected leg to push up, only to lower down.
| Level | Hold | Reps | Sets | How Often | Tips |
|---|---|---|---|---|---|
| Mild | slow 3-sec lower | 15 | 3 | 2×/day | Do this TWICE — once with a straight knee (targets gastroc) and once with a bent knee (targets soleus). Pain up to 5/10 during the exercise is acceptable and expected |
| Moderate | slow 3-sec lower | 10 | 2 | 1×/day | Start with both legs lowering together. Progress to single-leg when pain drops to 3/10 or less |
| Severe | slow 3-sec lower | 8 | 1 | every other day | Both legs only. If this is too painful, stick with seated heel raises (the exercise above) until your pain drops enough to try these |
How to progress: Bodyweight → add a weighted backpack (5 lbs at a time). Both legs → single leg. Work up to the full Alfredson protocol (3×15, twice daily). Once that's manageable, the Silbernagel protocol adds concentric (pushing up) and eventually plyometric (jumping) phases.
⚠ When to skip this: Do NOT do this with a suspected Achilles rupture. IMPORTANT: If your pain is at the insertion point (where the tendon attaches to the heel bone — insertional tendinopathy), do NOT let your heel drop below the level of the step. Modify to flat-ground heel raises only. Also avoid with an acute Jones fracture.
.webp)
Wall Calf Stretch — Gastrocnemius (Straight Knee)
This stretch targets the gastrocnemius — the big, powerful calf muscle that gives your leg its shape. It crosses both the knee and the ankle, which is why you stretch it with a straight knee. When this muscle is tight (a condition called equinus), it forces the front of your foot to work overtime with every step, contributing to heel pain, bunions, metatarsalgia, Achilles problems, and more. Loosening it up is one of the single most impactful things you can do for your feet.
What to expect: You should feel a noticeable difference in ankle flexibility within 2–4 weeks of daily stretching. Many patients report that heel pain and forefoot pressure begin to ease as the calf loosens. The clinical goal is at least 10 degrees of ankle dorsiflexion (the ability to pull your foot up toward your shin) — your podiatrist can measure this at your visit.
How to do it: Stand facing a wall with your hands flat at shoulder height. Step one foot back about 2 feet. Keep the back knee STRAIGHT and the heel firmly on the ground — this is the key. Lean gently into the wall until you feel a good stretch in the upper calf of the back leg. Keep your toes pointed forward, not turned out.
| Level | Hold | Reps | Sets | How Often | Tips |
|---|---|---|---|---|---|
| Mild | 30 sec | 3 | 1 | 3×/day | That's 90 seconds per leg, per session. It should feel like a firm, satisfying stretch — not pain |
| Moderate | 30 sec | 2 | 1 | 2×/day | Don't lean as far into the wall if the stretch is uncomfortable. Heel stays down no matter what |
| Severe | 20 sec | 2 | 1 | 1×/day | If standing is too much, try the seated version: sit with your leg out, loop a towel around the ball of your foot, and gently pull your foot toward you |
How to progress: Increase hold time to 45–60 seconds. Try slight toe-in and toe-out angles to stretch different parts of the muscle. Eventually, you can do this on a slant board for a deeper stretch.
⚠ When to skip this: Do not do this if you suspect an Achilles rupture (a sudden pop or snap in the calf). If you have insertional Achilles tendinopathy (pain right where the tendon meets the heel bone), do NOT stretch past neutral — stop before you feel the heel stretch. DVT (blood clot) suspicion: if your calf is swollen, red, and warm, see a doctor immediately instead of stretching.
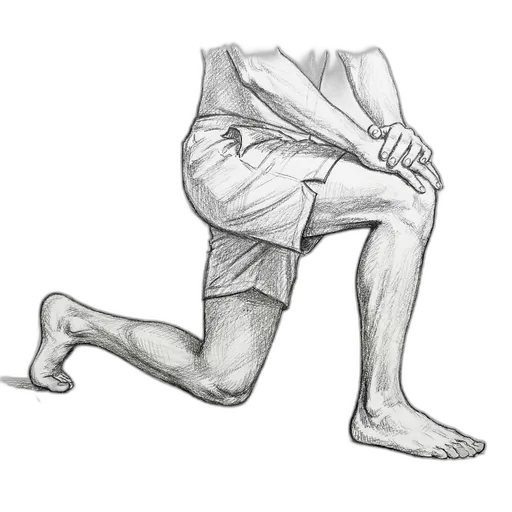
Half-Kneeling Dorsiflexion Mobilization
This mobilization targets the ankle joint itself — specifically the talocrural joint, where your shin bone meets your foot. Sometimes ankle stiffness isn't just tight muscles; the joint capsule itself gets stiff, especially after injury or immobilization. This exercise gently pushes the talus bone (your ankle bone) backward in its socket while improving dorsiflexion (the ability to bend your ankle upward). Think of it as "oiling" the hinge of a stiff door.
What to expect: You should notice improved ankle "bend" within 1–2 weeks. A simple home test: kneel in front of a wall, put your toes 4 inches from the wall, and try to touch your knee to the wall without lifting your heel. Track your progress by increasing the distance — 5 inches is good, 6+ inches is great.
How to do it: Kneel on one knee (a folded towel under the knee helps). Place the other foot flat on the floor in front of you. Keep that front heel firmly on the ground and gently drive the front knee forward over your toes — your knee should track over your 2nd or 3rd toe. You'll feel a deep stretch in the front of the ankle.
| Level | Hold | Reps | Sets | How Often | Tips |
|---|---|---|---|---|---|
| Mild | 5-sec oscillations or 30 sec sustained | 15 | 3 | 1×/day | Oscillate: gentle rhythmic push-and-release at end range. Like rocking a stiff door open a little further each time |
| Moderate | 5-sec oscillations | 10 | 2 | 1×/day | Smaller range of motion — don't force it to end range. Stop immediately if you feel pinching in the front of the ankle |
| Severe | gentle oscillations only | 8 | 1 | every other day | Try the seated version: sit with your foot flat on the floor and gently lean your knee forward over your toes. Skip this if the ankle is still swollen |
How to progress: Increase the depth of the lunge. Add a resistance band looped around the ankle (pulling backward) for a posterior glide mobilization — this gives the joint a mechanical advantage. Measure progress with the knee-to-wall test.
⚠ When to skip this: Skip with an acute ankle fracture. If you have a bone spur at the front of the ankle (anterior impingement), this may cause pinching — stop if you feel a sharp catch in the front of the joint. Wait for post-surgical clearance.
Active Standing Practice
This is something you can practice any time you're standing — in the kitchen, in line at the store, at your desk. Simply try to gently shorten your foot by lifting the arch without curling your toes. It's a subtle movement — no one will know you're doing it. But over time, it builds the small muscles inside your foot that support your arch from the inside.
How to do it: Stand with feet shoulder-width apart. Without curling your toes, try to gently pull the ball of your foot toward your heel — as if shortening your foot by half an inch. Hold 5 seconds, release. Repeat whenever you remember throughout the day.
When to See Dr. Patish
Don't wait on this one. PTTD is progressive — the earlier you intervene, the more options you have. If you notice your arch flattening on one side, if you can't do a single-leg heel raise without pain, or if your shoes are wearing unevenly, schedule an evaluation. Dr. Patish can stage the condition, fit you for supportive orthotics, and get you started on a targeted strengthening program before it progresses.
Frequently Asked Questions
Can exercises fix a flat foot from PTTD?
In Stage 1-2 (flexible flatfoot), exercises combined with orthotics can significantly improve arch support and reduce pain. The intrinsic foot muscles you'll strengthen in this program act like a built-in orthotic. In Stage 3-4 (rigid flatfoot), exercises help manage symptoms but can't reverse the structural change.
Do I need orthotics?
Almost always, yes — especially in the early stages. Orthotics support the tendon by controlling pronation and preventing the arch from collapsing further. Think of exercises as building internal support and orthotics as providing external support. They work best together, not instead of each other.
Need personalized guidance? Dr. Patish can evaluate your specific condition and adjust this program to your needs.




























